If you’re reading this, you’ve probably been trying to put together the puzzle pieces.
Maybe your child suddenly after an illness, a cold, strep, viral exposure, or even a vaccine. Maybe they started washing their hands until they’re raw, refusing to sleep alone, or raging in a way that feels completely unrecognizable. Maybe someone, another parent, a practitioner, or even Google at 2am, introduced you to the words PANS or PANDAS, and suddenly, everything started to make a little more sense. I’ve been there.
And now you’re wondering:
“What do I do next?”
“Who do I call?”
“Is this really it?”
You are not alone.
Thousands of families have walked this road, often after being dismissed by pediatricians and specialists, misunderstood by schools, or second-guessed by spouses and relatives, who think it’s just a behavioral or discipline problem. That is often the most frustrating part of this journey: you’re not only trying to care for your child, you’re trying to convince others that what you’re seeing is real.
This post is here to help.
This is your starting place. Let’s walk through it, step by step.
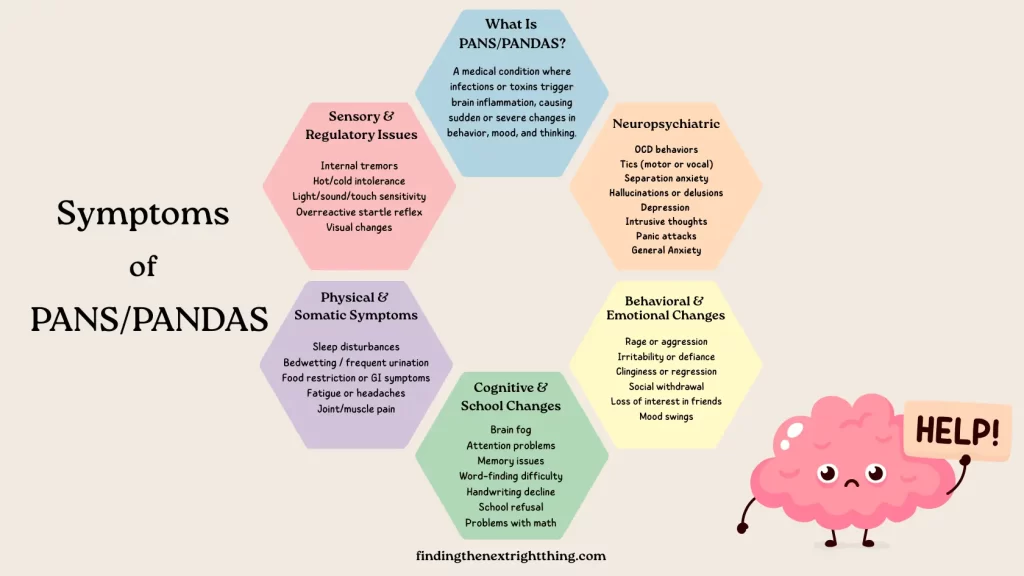
What are PANS/PANDAS?
PANS = Pediatric Acute‑onset Neuropsychiatric Syndrome; PANDAS is the subgroup triggered by streptococcal infections. Both are neuroimmune conditions where an infection, or sometimes environmental trigger, causes the immune system to attack the brain. The result is a sudden and dramatic onset of symptoms like OCD, anxiety, rage, tics, eating restrictions, and sleep disturbances. PANDAS is specifically triggered by strep, while PANS can be triggered by other infections (like Mycoplasma, Lyme, Bartonella or viruses), mold, toxins, or even trauma.
Not sure if what you’re seeing is PANS or PANDAS?
If you’re still piecing things together and want a clearer understanding of the signs and symptoms of PANS or PANDAS. Be sure to check out this post on the most common symptoms of PANS and PANDAS, where I break down the red flags, patterns, and what parents often notice first. It’s a helpful place to start if you’re trying to connect the dots.
Step 1: Trust What You're Seeing & Start a Symptom Journal
Before anything else, you need to do two things:
Trust yourself.
Start documenting.
If you’re here, it’s likely because you’ve noticed something in your child that doesn’t feel “normal.” Not just quirky. Not just anxious. Different. Sudden. Deeply dysregulated. You’ve watched your child shift, sometimes overnight, and something in you said: this isn’t right.
Why You Need a Symptom Journal
PANS/PANDAS symptoms can wax and wane, what’s intense today might ease up tomorrow. A symptom journal helps you:
Track patterns (especially in relation to illness, food, sleep, or stress)
Spot early signs of flares before they escalate
Provide clear documentation to providers
- Notice improvements you might otherwise miss
And if you’re dealing with skeptical doctors or confused family members, having a written timeline of symptoms can help.
What to Track
You don’t need to make it complicated. Start simple:
Date & time of day
Emotional symptoms (rage, anxiety, crying, panic)
Physical symptoms (tics, handwriting changes, sleep issues, urination frequency)
Triggers (exposure to illness, mold, sugar, stress, school, etc.)
Interventions tried (ibuprofen, curcumin, herbs, supplements)
Any new exposures (viruses, foods, school events, medications)
Step 2: Talk to Your Pediatrician + Ask for Baseline Labs
Once you’ve started tracking symptoms and you have a growing suspicion that something deeper is going on, the next step is having a conversation with your pediatrician. This can be a turning point, or a frustrating roadblock.
Many pediatricians are not yet trained to recognize PANS or PANDAS. Some are open and curious, others more skeptical, and think that a child only has PANS/PANDAS if they fit exactly in certain parameters and lab tests. Either way, it’s okay to advocate for your child and ask for a baseline workup to rule out potential triggers and inflammation. You don’t need to convince your pediatrician of a PANS/PANDAS diagnosis right away. Your goal at this stage is to request labs. You’re simply asking to rule things out.
What to Say to the Pediatrician
Here’s a simple, non-confrontational script you can use:
“We’ve noticed some changes in our child—OCD behaviors, anxiety, rage, sleep issues, _________… We’re tracking symptoms and trying to understand what might be triggering them. I’ve been reading about PANS and PANDAS, and I’d like to start by checking some labs to rule out infections or inflammation. Could we order a basic panel? Do you have any other patients with PANS/PANDAS?”
If your pediatrician says yes—great! If they seem unsure, you can offer a short lab list (see below), or ask for a referral to someone who specializes in autoimmune or neuroimmune disorders.
Our current pediatrician’s office (who we found after our own very uninformed pediatricians) has a PANS/PANDAS entry on their standard lab slips. If you have a pediatrician’s office like that, you are winning!
If they outright refuse or dismiss your concerns, don’t panic. It’s not the end of the road. There are other ways to get there.
(But, if your child is in a severe state or in a flare and you believe it is PANS or PANDAS you need to consider finding another pediatrician, more about that below.)
Basic Labs to Request
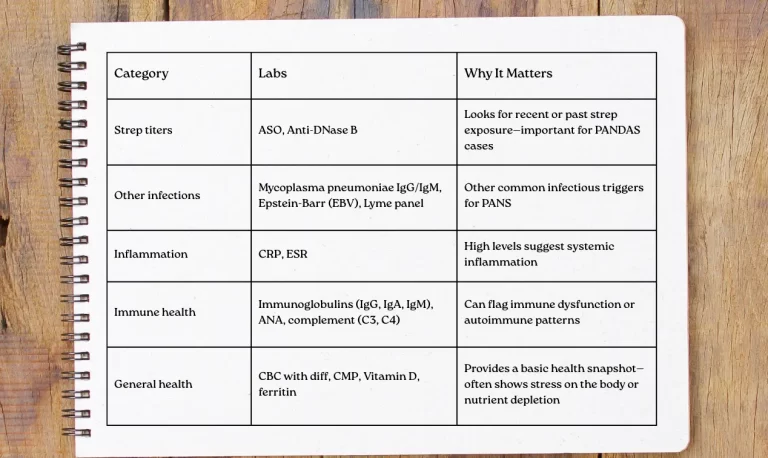
Once you receive the results log them in your symptom and treatment journal. If Vitamin D is low, start supplementing!
Don’t be discouraged if the labs come back “normal”—normal results do not rule out PANS or PANDAS. In our case, standard lab work for our oldest child was always within normal range, but he still tested positive on the Cunningham Panel. He was also positive for Bartonella through Igenex, even though he was negative for Bartonella through LabCorp.
The Cunningham Panel is currently one of the most reliable tools we have to support a PANDAS diagnosis. That said, it’s not definitive, and it tends to be more accurate for PANDAS (strep-triggered cases) than for broader PANS presentations, which can be triggered by other infections or environmental factors. There is a new test, Neural Zoomer, that is supposed to be more accurate for PANS, but it’s currently only used by functional or integrative type doctors. And, both are very expensive, and not necessary or even helpful at the initial stage when you just need to stabilize.
Step 3: First Line Interventions—Conventional + Natural Support
Always talk to your doctor before starting these interventions.
If your pediatrician is open to PANS/PANDAS as a possible cause, or at least sees the logic in trying to reduce inflammation, you could request that they start with:
Antibiotics
In many PANDAS cases, a trial of antibiotics (like amoxicillin, azithromycin, or Augmentin) can reduce symptoms.
Why? Because:
They may treat an underlying infection (like strep or Mycoplasma)
Some antibiotics (like azithromycin) have anti-inflammatory properties and can help restore tight junction proteins to reinforce the integrity of the BBB
A dramatic improvement on antibiotics can help confirm immune involvement
Not every child will respond to antibiotics—but some show noticeable improvement in OCD, rage, or sleep within 72 hours.
But, if this was not your child’s first flare, or if they’ve been undiagnosed/untreated for a long period of time, one short course of antibiotics is probably not going to bring them back to baseline. You may see improvements, but it will likely take much longer and more interventions to bring them to baseline. So if a pediatrician tells you that because a 10-day course of antibiotics didn’t take him back to baseline it’s not PANDAS, they are not well informed or educated about PANDAS. This was what I was told by our former pediatrician and it still irritates me. Especially because he was in that chronic state because they dismissed me for over a year about PANDAS as a possibility for his symptoms. So don’t be me, keep pushing, find a pediatrician that is known as PANS/PANDAS friendly.
Ibuprofen
This simple OTC NSAID is one of the top defenses in a flare. If a course of Ibuprofen helps calm the symptoms, it’s actually an indication that you’re dealing with PANS/PANDAS (It was for my twins). It doesn’t mean it’s not PANS/PANDAS if Ibuprofen doesn’t help for a lot of different reasons, but if rage, anxiety or OCD is calmed by an anti-inflammatory, then there is likely neuroinflammation involved.
In our experience, ibuprofen has helped to:
Calm rages
Reduce obsessive thoughts
Improve sleep
Ease sensory overload
Things to Consider:
Not all kids tolerate it well. Always talk to your provider first. Some may have gut sensitivity or react poorly, especially if your child has a history of reflux, gastritis, or GI bleeding.
Use in short bursts, not long-term unless advised by your doctor. There are more risks with long-term use. Ours advises twice a day for 7 or 10 day courses. Always give with food, monitor for side effects and talk to your doctor.
Benadryl
Benadryl can sometimes calm symptoms in the middle of a flare—especially when histamine is involved.
Why it can help:
Acts as a mast cell stabilizer, reducing the release of histamine and inflammatory cytokines
Can calm the nervous system in children who are overstimulated, anxious, or in rage cycles
May improve sleep during a flare when cortisol and histamine are elevated at night
When to consider it:
Rage or aggression that seems to appear “out of nowhere”
A flare triggered by environmental exposure (pollen, mold, perfumes, food dyes)
Sleep disruption that looks allergic or restless
Some kids may get sleepy; others (especially if overmethylated or very sensitive) may get wired or agitated—track reactions carefully.
If Benadryl helps, that’s often a sign to explore deeper histamine, mast cell, or mold-related issues.
Steroids (Short-Term Burst)
For some kids, a short course of oral steroids, often called a “burst” can dramatically reduce inflammation during a severe flare. Steroids like prednisone work by suppressing immune activity and calming microglial activation in the brain, which can sometimes help reset the system when nothing else is touching the symptoms.
A steroid burst is usually considered when symptoms are on the severe end of the spectrum or aren’t getting better after other methods, like when a child is stuck in a loop of nonstop rage, anxiety, or debilitating OCD, and antibiotics and Ibuprofen aren’t working. For some families, it’s the only thing that brings their child back to baseline.
That said, steroids are powerful and come with risks. They’re not for everyone. Some kids get relief; others get “Roid Rage,” one of mind included.
If your provider recommends a burst, ask about tapering protocols and whether to use alongside antibiotics or anti-inflammatories. And keep tracking symptoms. It’ll help you understand if steroids are helpful for your child, or if they add to the chaos. In our experience, the full effects of the steroids weren’t experienced until after they finished the burst.
When your child is in a flare, or riding the edge of one, reducing inflammation and calming the nervous system is essential. While medications like ibuprofen and Benadryl have their place, many families find plant-based compounds and nutraceuticals to be just as effective, sometimes more so, especially when used preventatively or alongside root-cause work.
Below are some of my favorite dual- or triple-duty tools: they don’t just target one system, they support inflammation, histamine, detox, and the brain at once.
Natural Anti-Inflammatories + Nervous System Support
Top Natural Anti-Inflammatories
Curcumin
The active compound in turmeric, curcumin is a broad-spectrum anti-inflammatory with strong antioxidant properties. It blocks NF-kB and COX-2—two key inflammatory pathways involved in flares. Curcumin is well-known as being helpful in reducing neuroinflammation, joint pain, mast cell activity, and calming gut irritation.
Look for liposomal, phytosomal (Meriva®), or BCM-95 forms for better absorption.
Pairs well with Resolvins, or omega-3s for deeper inflammation control.

Resolvins (SPMs)
Specialized Pro-Resolving Mediators (SPMs) are derived from omega-3 fatty acids and signal the immune system to turn off inflammation once it’s done its job. They don’t just block inflammation—they help the body resolve it. It can work wonders for persistent, smoldering inflammation like in chronic flares or post-viral neuroinflammation. We use and love Dr. Crista’s formula. They are a small gel capsule, that even my ARFID, strong gag-reflex kid doesn’t have a problem.
Pycnogenol (French Maritime Pine Bark Extract)
Pycnogenol is a powerful antioxidant and natural anti-inflammatory that also boosts blood flow to the brain and improves executive function. Supports cognitive clarity, reduces oxidative stress, and has been shown in studies to improve ADHD symptoms in children. I like to give this herb before school! Also helps regulate glutamate and dopamine, key neurotransmitters disrupted in PANS/PANDAS.
Feverfew + Perilla
Note: You do not have to take these two together, but if you have any allergies feverfew can make you itchy! It’s a powerful anti-inflammatory and if you combine with perilla, it balances out the feverfew and avoids the itchies for us.
Feverfew is traditionally used for migraines, it works by inhibiting prostaglandins and calming blood vessel reactivity.
Perilla leaf is one of my favorites and a true multitasker: anti-inflammatory + mast cell stabilizer + histamine regulator. Perilla, on its own is excellent for histamine-driven flares, seasonal allergies, food reactivity, or sensory overload.
Aloe (Inner Leaf Gel or Juice)
Aloe is often overlooked as an anti-inflammatory but it does triple-duty for PANS/PANDAS:
Gut Soother – Calms irritation, rebuilds the gut lining, and promotes healing from leaky gut
Gentle Binder – Binds mycotoxins in the gut without disrupting nutrient absorption
Mild Antihistamine – Aloe contains compounds that may reduce histamine release and calm mast cells
Great to use during gut healing phases or after mold exposure
Go deeper on natural anti‑inflammatories in the Herbal Guide: Inflammation Support.
Natural Nervous System Calmers
These herbs aren’t just calming—they each come with secondary actions that make them ideal for complex kids with overlapping inflammatory + histamine + immune challenges.
Gotu Kola
Gotu Kola is a traditional Ayurvedic nervine and nootropic that promotes calm alertness. It’s known as a “brain tonic.” Gotu Kola enhances parasympathetic tone (rest/digest), reduces endotoxin-related neuroinflammation, and supports blood-brain barrier integrity.
Also supports cognition and memory—ideal for recovery phases after flares.
Albizia
Albizia is known as the “Tree of Happiness” or “happiness bark” for its gentle uplifting calming effect. It has a mood stabilizing effect, soothing emotional dysregulation and irritability. It’s also a natural antihistamine, calming histamine related agitation.
Ashwagandha
Ashwagandha is a foundational adaptogen for stress recovery and immune regulation. It balances cortisol, calms the HPA axis, and supports mood, sleep, and inflammation reduction. It also functions as a neuroinflammatory modulator—targeting cytokines like IL-6 and TNF-alpha.

Targeted Support for OCD + Rage in PANS/PANDAS
Herbs can calm the nervous system, but some symptoms like OCD looping, intrusive thoughts and rage could often use extra support. These nutraceuticals work on neurotransmitter balance and neuroprotection.
As always go slow, these work great for some kids and others do not tolerate them well.
Inositol
Neurotransmitter Support • OCD + Anxiety Relief • Mood Stabilizer
Inositol helps regulate serotonin and dopamine, two key neurotransmitters involved in OCD, anxiety, and mood swings. Research supports its use in OCD, particularly in higher doses, and many PANS functional medicine doctors use it as a natural alternative or complement to SSRIs.
NAC
Glutathione Precursor • Detox + Neuroinflammation Support • OCD Modulator
NAC is a precursor to glutathione, the body’s master antioxidant, and plays a major role in detox and neuroinflammation. reduction. It also modulates glutamate—the excitatory neurotransmitter often elevated in kids with OCD, anxiety, and PANS flares.
Low-Dose Lithium
Mood Stabilizer • Neuroprotective • Rage + Impulsivity Support
This is NOT the pharmaceutical version—lithium orotate is a low-dose mineral supplement. It stabilizes volatile mood swings, calms limbic overactivation, and supports neuronal repair after prolonged flares. Lithium also helps modulate glutamate and reduces brain inflammation in the prefrontal cortex—important in rage and aggression cycles.
Saw Palmetto
Androgen Modulator • Anti-inflammatory • Aggression Support
Saw Palmetto is best known for hormonal balance, saw palmetto is emerging in PANS/PANDAS care for its ability to reduce aggression and rage. It also has mast cell stabilizing and anti-inflammatory properties.
Herbs can interact with medications. Always consult your provider, especially if your child takes prescription drugs or has a history of autoimmune disease.
Don't Overlook Minerals: Magnesium, Zinc and Trace Minerals
Minerals are like spark plugs for the body; they power nearly every biological process. Adding core minerals—especially magnesium, zinc, and trace minerals, can be significant for these kids. These minerals are often the first to be depleted during inflammation, stress on the body, picky eating, or long-term illness.
And they’re some of the most powerful tools you can start with. Read more about Minerals in the Herbal Guide.
Magnesium- The Calming Mineral
Magnesium is one of the most essential—and most commonly depleted—minerals in the body. It’s involved in over 300 biochemical reactions, and the majority of Americans are either deficient or insufficient. For kids with PANS/PANDAS, the need is even higher. Their bodies are under constant stress—whether from inflammation, immune activation, or emotional dysregulation—and they tend to burn through magnesium more quickly than the average child.
Magnesium is known as the “calming mineral” as it can ease anxiety, irritability, improve sleep, relax muscles, support detoxification, and help regulate neurotransmitters. There are many, many different forms of magnesium.
Common forms of Magnesium for PANS/PANDAS kids:
Magnesium Glycinate – is one of the gentlest and most calming forms, well-absorbed and ideal for reducing anxiety and supporting sleep.
Magnesium Threonate – helpful for cognitive issues, or emotional volatility, as it crosses the blood-brain barrier. This is the form we most often take.
Magnesium Malate – can be helpful if dealing with fatigue or sluggish mitochondria because it can have an energizing effect and support ATP production
If your child has gut sensitivity or trouble swallowing capsules, start low and slow. Transdermal options like magnesium oil sprayed on the feet or Epsom salt baths can be a great first step. You can also find transdermal patches. These allow the body to absorb magnesium through the skin, bypassing the digestive system altogether, which can also be helpful if a child is not properly absorbing nutrients in the gut.
Zinc for Immune Function and Appetite Stimulant
Zinc can also be very supportive for children with PANS/PANDAS. Zinc supports immune function, wound healing, neurotransmitter regulation, and detox pathways—but it also plays a critical role in stimulating appetite. Zinc is commonly low in PANS/PANDAS kids due to inflammation. You can start with food sources from beef, pumpkin seeds or sunflower seeds or try a low-dose zinc supplement.
Note, zinc and copper work together, too much of one can suppress the other.
Trace Minerals or a Multi-Mineral
My functional medicine practitioner has me use MiniRex, but we also rotate in BEAM Humic Acid, Seeking Health Trace Minerals, and sometimes Shilijat. I like to rotate in different forms to keep the support well-rounded.
For kids who are sensitive to powders or capsules, electrolyte mixes with added minerals (like LMNT, Ultima, Just Ingredients, or Beam) are a great way to sneak minerals into their water or smoothies.
You've Taken the First Step
You’ve already done one of the hardest things: recognized that something deeper is going on with your child, and started taking steps to understand it.
You’ve begun tracking symptoms. You’ve opened the conversation with your pediatrician (or you’re preparing to). You’ve explored the first tools that can reduce inflammation, calm the nervous system, and begin easing your child’s suffering.
For many families, just reaching this point can take months, or years (in our case).
But you’re here now. You’re moving forward. And there is a path ahead.
What Comes Next
In Part 2 of this series, we’ll walk through what happens after the initial groundwork is in place:
How to choose the right type of provider (and what to do if you can’t find one)
How to clean up the “terrain” so your child’s body can begin to heal
The foundational support systems that help regulate the immune response, reduce flare triggers, and support long-term recovery
The bigger picture: how to build a sustainable, layered, root-cause healing plan
It’s not about finding one magic pill. It’s about learning to support your child’s system with wisdom, patience, and a plan.
You don’t have to figure it all out today. Just keep going. Keep learning. Keep trusting what you see in your child.
Click here to read Part 2: Building Your Child’s Healing Roadmap
(or drop your email below and I’ll send it straight to your inbox when it goes live)
When to Seek Urgent Care
If your child develops self‑harm thoughts, severe dehydration, refusal to eat or drink, or completely lost functional baseline — seek urgent evaluation.
Hi, I’m Brooke. I’m an herbalist and mom to three kids with PANS/PANDAS. Everything on this site comes from years of research, lived experience, and talking with other families walking a similar road.
If you’re just getting started, begin with What is PANDAS? to get familiar with symptoms and warning signs. Then head to So You Suspect PANDAS, Now What? for practical steps you can take right away.
You’ll also find targeted guides on things like:
Detox: how to support the body’s drainage and clearing pathways
Anti-Inflammatory Herbs: for calming flares and easing symptom intensity
Root Cause: Toxins: common environmental triggers worth addressing
The Root Causes Guide and Main Herbal Guide: to help you connect the dots and build a layered plan
You don’t have to learn everything at once. Just keep going. Keep asking questions. And, keep your hope! You’ll get there.
~Brooke

No comment yet, add your voice below!